A malignant tumor differs from other types of tumors and diseases in that its cells are similar to healthy cells of the body. Therefore, scientists face a difficult task: to distinguish between cells and destroy only infected ones. Throughout the story, doctors had different ideas on how to do this. Today,
Atlas will talk about how cancer has developed and how cancer is treated today.
 Illustrations: Michael Kowalski
Illustrations: Michael KowalskiHippocrates Humoral Theory
Until the 18th century, cancer was difficult to study: the appropriate equipment had not yet been invented, the church forbade an autopsy, and plague and smallpox claimed more lives and attracted attention. Therefore, since ancient times, few records of malignant tumors have reached us, but they still exist.

The first mentions of cancer are found in Edwin Smith's papyrus, the medical text of Ancient Egypt, which dates back to the 16th century BC. This
papyrus can be looked through and read. Case number 45 just describes a malignant tumor. It also notes that there is no treatment method.
Hippocrates (400 BC) was the first to distinguish benign and malignant tumors. He believed that the human body contains four humors, or fluids - blood, mucus, yellow and black bile - and any imbalance leads to diseases. It was believed that the cause of malignant tumors - the accumulation of black bile in a certain place. Hippocrates noted that without treatment, patients can live longer: black bile has already spread throughout the body and cannot be removed.
Of course, there is no black bile in the human body, but the idea of spreading the tumor throughout the body turned out to be true. Malignant cells eventually separate from the tumor and metastasize.
Doctors and healers have used humoral theory for more than 1,300 years. During this period, autopsies were prohibited for religious reasons, which limited the study of tumors. The available methods of treatment in ancient times and the Middle Ages were surgery, cauterization, bleeding and rites.
The first surgical intervention
Surgery is one of the most ancient branches of medicine. However, in medieval times, interventions did not always lead to the desired results due to the large loss of blood, the high risk of infection after surgery, and the absence of antiseptics.
GalenRoman doctor Galen (130–200 AD) wrote about the surgical treatment of breast cancer at an early stage, but did not consider this method effective for the treatment of large and “hidden” tumors. He adhered to the humoral theory and assumed that black bile cannot be completely removed from the body. This approach saved many lives: in the Middle Ages, patients often died during surgery or because of complications after it.
Cancellation of humoral theoryAfter the lifting of the prohibition on autopsies in the 16th century, Andreas Vesalius compiled the first anatomical reference book of the human body, and a century later Matthew Bailey described the structure of various pathologies. The humoral theory had to be reconsidered, as scientists did not find any black bile.

In the 17th century, surgical methods to remove tumors began to develop. The German surgeon Wilhelm Fabri, during an operation to remove breast cancer, excised the tumor along with enlarged lymph nodes, and the Dutch surgeon Adrian Helvetius performed a mastectomy, complete removal of the mammary gland. A few years later, he wrote about one of the cases: “Since then, the patient has fully recovered. The pains have completely stopped, the scars have healed, and she is enjoying the same state of health that she had before the cancer. ”
In the 1850s, the German scientist Rudolf Virkhov discovered uncontrolled cell division in tumors. He called this phenomenon neoplasia, and his main work, Cellular Pathology, became the basis for understanding the causes of cancer.
Pain relief and antisepticIn 1846, anesthesia was invented. This solved the problem with pain, because before that people had to experience an operation in consciousness. And in 1867, French physician Joseph Lister discovered that ointment based on carbolic acid acts as an antiseptic and promotes wound healing after surgery.
Anesthesia and the first antiseptic expanded the possibilities of surgery, and operations began to be carried out everywhere. However, in some cases, tumors appeared again. Then surgeons began to expand the scope of interventions, which eventually led to the emergence of a method of radical surgery.
Radical surgerySurgeon William Halsted thought that the more tissues removed during surgery, the less likely there would be a relapse. The conclusion is not entirely correct, since the malignant cells could have spread throughout the body and metastasize to other tissues before the operation.

Only in the 1970s was it proved during clinical trials that less extensive surgeries are as effective as radical ones. Unfortunately, by this time, radical mastectomy had gained a lot of popularity and was considered practically the only correct method for treating breast cancer.
ModernityIn the 1990s, surgeons minimized interference with healthy human tissue. Today, operations are divided into two types: open and minimally invasive. For open surgery, the doctor makes a large incision to remove the tumor, unhealthy tissue, and possibly lymph nodes.
For a minimally invasive surgery, the doctor makes several small incisions, finds the tumor with a thin tube with a camera (laparoscope) and removes the tumor with tools through another incision. After this operation, the patient recovers faster.
Radiation therapy
In the late 19th century, scientists paid attention to the ability of X-rays to kill malignant cells. At that time, no one had yet guessed how detrimental the radiation affected healthy tissue.
X-ray tubesX-rays were discovered in 1895, simultaneously with the development of radical surgery. A year after this, a young doctor, Emil Grube, noticed how the skin and nails of people who worked with radiation sources were destroyed. He suggested that the rays kill the tumor cells, and was the first to use radiation therapy to treat cancer.
The method quickly gained popularity: new clinics offering radiation therapy opened in Europe and the USA. It was effective in cases when the tumor did not have time to spread to other organs.
The idea of using radiation was excellent, but it did not take into account two significant minuses of the X-ray tube: inhomogeneous radiation flux and insufficient penetrating power. Most of the dose is absorbed by other tissues or scattered. Thus, X-rays increase the number of mutations in healthy cells, which leads to the formation of new tumors. This option cannot be considered a suitable treatment.
RadiumIn 1902, scientists Pierre and Marie Curie discovered the radioactive properties of radium. At first glance, this substance penetrated deeper X-rays and gave more opportunities for treatment. For 10 years after the discovery of radium, many doctors and scientists who did not know about the danger of radiation developed various malignant diseases. This continued until the first dosimeters and standards for measuring radioactive radiation appeared.
Electron accelerator and radioactive cobaltIn 1940, Donald Kerst assembled the betatron, a cyclic electron accelerator. The device emits particles with high energy and penetrating ability, so when using it, few scattered rays arise. In 1951, Swedish neurosurgeon Lars Leksell developed the Gamma Knife. It has several sources of radiation of radioactive cobalt and gives a uniform beam of high energy. Betatron and gamma knife are successfully used to treat tumors today.

Radiation destroys the DNA of cells directly or indirectly. In the second case, the water that is contained in the cells is converted into free radicals - charged particles that damage DNA. Radiation does not understand which cells to destroy, healthy or malignant, so the devices require careful adjustment so that the peak of the dose falls to the desired depth.
ModernityToday, oncology uses x-rays, gamma rays and charged particles. They can enter the body and act on malignant cells through a special device or come from radioactive material placed in the patient’s body next to the tumor (brachytherapy).
There is also a third type of radiation therapy - systemic. The patient is injected with a radioactive liquid, such as iodine, which finds and kills the tumor cells. But in this case it is difficult to take into account the exact amount of isotope that the body absorbs, and the dose may be harmful.
Chemotherapy
Surgery and radiation therapy were used to treat solid tumors that do not develop from the cells of the hematopoietic system. Nobody knew how to treat lymphomas and leukemia.
Mustard gasThe idea of using toxic substances to treat these diseases arose after the First World War. At this time, mustard gas - mustard gas was used as chemical weapons. He burned the skin and mucous membranes, and also killed leukocytes: they were virtually absent from the wounded.
Scientists have wondered if mustard gas can cure lymphoma - a tumor of lymphatic tissue. In this disease, the lymphocytes divide uncontrollably and disrupt the functioning of the lymph nodes and other organs, so the reduction of lymphocytes seemed like the right decision. In 1942, after animal studies, 10 doses of mustard gas were injected intravenously into a patient with lymphoma. The number of lymphocytes quickly fell, and the tumor decreased, but later began to grow again. This meant that the therapy had an effect, but the dose was not enough for complete recovery.
Remission occurred because mustard gas belongs to the group of alkylating agents that destroy the DNA of cells and prevent them from sharing. But then they knew nothing about it.
 Methotrexate precursor
Methotrexate precursorIn 1947, physician Sydney Farber showed that a derivative of folic acid, ametopterin, suppresses the development of acute leukemia in children, which is characterized by the uncontrolled division of white blood cells. This drug was the precursor of methotrexate, which is used now.
The bone marrow biopsy results of patients after treatment with ametopterin were normal. Chemotherapy prolonged the life of children up to 6 months, but then the disease returned. Farber threw all his strength into finding a cure that could cure leukemia completely. Then it was difficult to assume that you need to use several toxic substances at once, and not just one.
In 1950, Gertrude Elion developed the drug 6-mercaptopurine (6-MP), which quickly received permission for use in children with leukemia. After him, the doctors again observed a short remission.
Combination ChemotherapyLater randomized clinical trials were conducted, during which it became clear that using two drugs instead of one prolongs remission and improves the prognosis.
In 1956, Dr. Min Chiu Lee clinically confirmed that a combination of four drugs cured metastatic choriocarcinoma in pregnant women. The National Institute of Oncology at first regarded these actions as aggressive and unnecessary treatment of patients, and the scientist was removed from work. Only later it became clear that only those women survived who had undergone the full course of treatment for Li. This was the first case of a complete cure with chemotherapy.
Adjuvant ChemotherapyIn the 60s and 70s, scientists tried to use chemotherapy as an additional treatment for breast cancer after surgery. Surgeons reluctantly went to clinical studies: no one wanted to deal with additional side effects in patients. But they were wrong.
In fact, any tumor is a systemic disease. Malignant cells spread throughout the body, even in the early stages, in the form of micrometastases. They remain in the body even after the removal of the tumor, so local treatment is not enough. It is necessary to systematically affect the disease with the help of drug treatment. For example, adjuvant therapy (a course of chemotherapy after surgery) reduces the risk of relapse and death.
Several studies have shown a positive result of adjuvant chemotherapy for the treatment of breast cancer and colorectal cancer. Also in 1974, a positive effect was proved in case of metastatic testicular cancer, and chemotherapy began to be used to treat solid tumors.
Chemotherapy drugs stop and slow down cell division. During the course of treatment, those cells that quickly divide die. It is not only malignant cells, but also healthy, which leads to side effects: hair loss, nausea, susceptibility to infections.
Immunotherapy
Immunotherapy is a relatively new type of cancer treatment. It is based on the use of drugs that train the patient's immune cells. This was made possible by the discovery of the structure of DNA, the study of the characteristics of malignant cells and cells of the immune system.
Coley's VaccineIn 1891, William Kohli noted that cancer patients who had scarlet fever or erysipelas had remission. After that, he began to inject patients with the last stage of cancer streptococcal bacteria. The tumor decreased, but the patients died from the infection. Then Kohl heated the vaccine and injected patients with dead streptococci.
The result for that time was impressive: the patients recovered and lived for several years. However, Kohl's vaccine was not widely available. Scientists could not explain the mechanism of how bacteria act on a tumor, and the risk of infection was high. All were much more interested in chemo and radiation therapy.
In 1976, the BCG vaccine, which was used to prevent tuberculosis, was successfully used to treat bladder cancer. It activates the immune system and helps the body fight this type of cancer.
Monoclonal antibodiesIn 1975, Georges Köhler and Cesar Milstein published an article about a method for obtaining a cell tumor cell hybrid and a lymphocyte. The hybridoma technology makes it possible to detect antigens characteristic of tumors of certain tissues, to obtain antibodies to them and to use them for diagnosis and typing of tumors. Such antibodies are called monoclonal: they are produced by clone immune cells that originate from a single parent cell.
Other types of antibodies mark cancer cells to make it easier for the immune system to find and destroy them.
In the late 1990s, the FDA approved the first therapeutic monoclonal antibodies, rituximab and trastuzumab. The first is for the treatment of lymphoma, and the second is for breast cancer.
In 2010, Stephen Rosenberg announced the success of therapy with chimeric antigen receptors. It is based on the genetic modification of the patient's T-cells for the treatment of a malignant tumor.
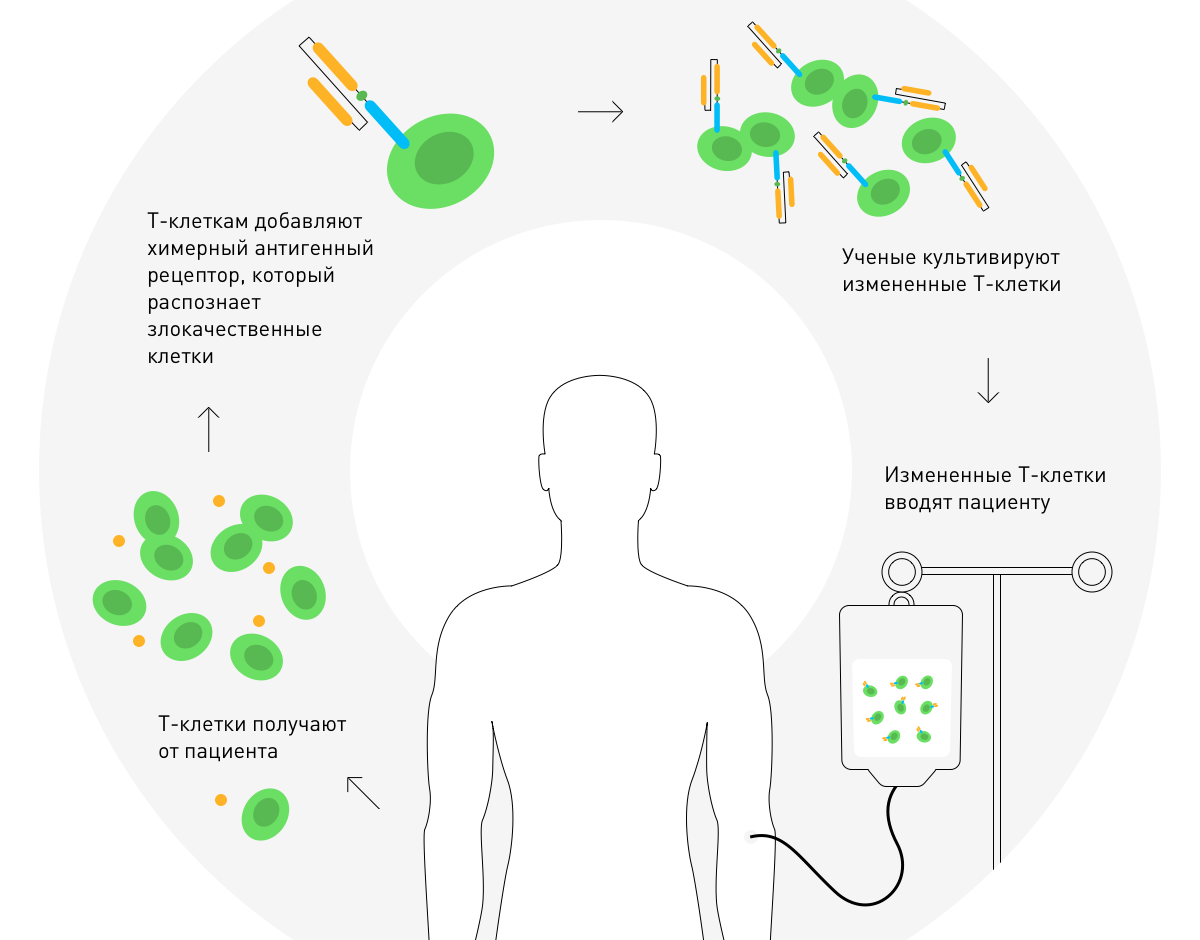 Cytokines
CytokinesAnother method of immunotherapy is the introduction into the muscle or vein of cytokines, biologically active proteins that regulate the immune response. Interleukin-2 helps the cells of the immune system to divide faster, and interferon helps fight viral infections and malignant tumors.
Control pointsAnother promising direction is the effect on immune checkpoints, which suppress the response of the immune system. Scientists have learned to block control points on T-cells, which helps the immune system to recognize and attack malignant cells. This method has already been approved by the FDA for the treatment of cancer.
You can choose the optimal treatment using molecular diagnostics. Scientists are researching a patient's surgical material or biopsy to identify mutations in proto-oncogenes and suppressor genes. The set of mutations is individual for each tumor, so treatment must be personalized. The next time
Atlas will talk in detail about molecular diagnostics.