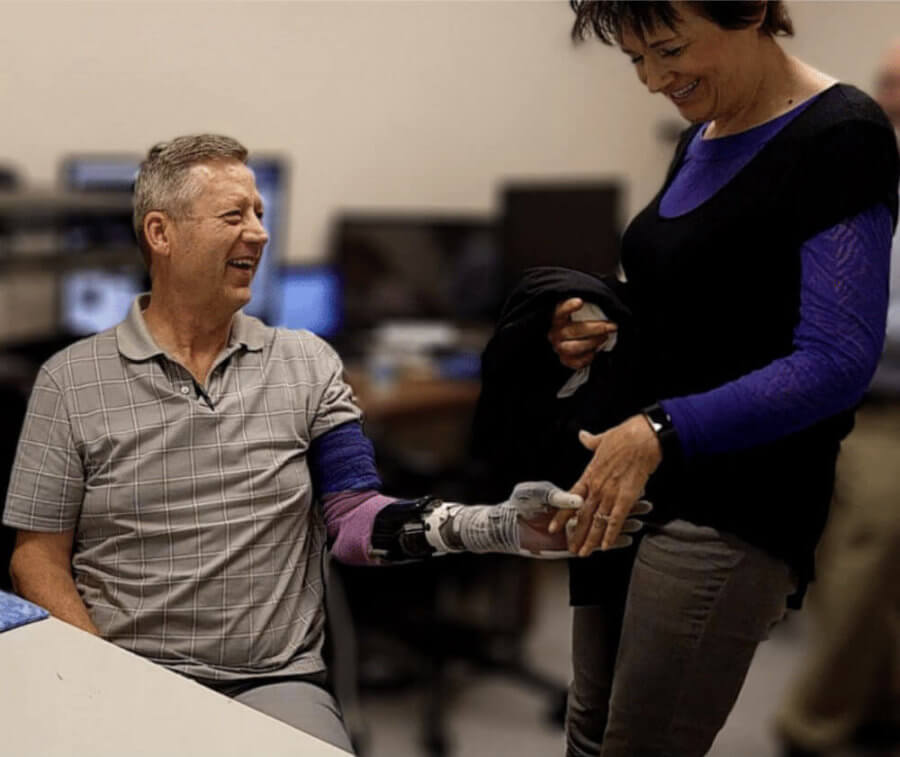
 Kevin Walgamot holds and feels his wife's hand again with an experimental robotic arm. Photo: Jacob George and co-author, Laboratory Doctor Greg Clark, University of Utah.
Kevin Walgamot holds and feels his wife's hand again with an experimental robotic arm. Photo: Jacob George and co-author, Laboratory Doctor Greg Clark, University of Utah.When Kevin Walgamot stretched, he took his wife by the hand, and his face broke into a huge smile. For the first time in 14 years, he could feel her soft fingers pressed tightly against the palm of the prosthesis.
David is testing a new interface that easily combines movement and sensation. What is the purpose? To replace the feeling of “alienity” of a robotic prosthesis with something intuitive and natural as part of oneself.
Implanted directly into the remaining nerves of Kevin's lost forearm, the interface translates thoughts into electrical signals that set the deft robotic arm in motion.
But this is not all: it also receives information from sensors on a robotic arm and sends it back to the brain through two implanted high-density, electric arrays. In the brain, electrical impulses are transformed into a sense of pressure, vibration and movement — sensations that come as if from their own missing limb.
It is this closed loop from thought to motion and then to sensory feedback that makes the device special.
“People often think of touch as a solitary feeling, but in fact it also includes other senses, such as pressure, vibration, temperature, pain, etc. The high resolution of our device allows us to activate these contact subclasses in isolation (i.e. pressure without vibration and pain) in a certain part of the arm. ”Says
Jacob George , who helped develop the interface at the
University of UtahUnlike previous generations of interfaces that transmit only about 20 sensations - for example, participants can feel only pressure, the new system restores 100 unique sensations with subtle differences.
And this radically distinguishes the interface.
George explains: “Our participants controlled prostheses with thought before that. They also felt the sensation of their missing hand earlier. But combining both approaches, adding feedback is a completely different experience. Suddenly the hand becomes alive again. ”
Prosthetics Problems
VideoResearchers at the University of Utah are developing an experimental robotic arm that is controlled by reading nerve impulses.Kevin is one of 1.6 million people in the United States who have had an amputation.
“Having lost a limb, you not only lose physically a part of yourself, you also lose a part of the spiritual component,” says George.
Depression and anxiety appear. Some patients even experience phantom pain, burning sensation, seemingly emanating from their amputated limbs, and do not respond to ordinary painkillers.
“Our participants described the loss of a hand as the loss of a family member who has to go through every day,” said George.
It is this “emotional beast” that is extremely difficult to tame. One of the reasons is that modern prostheses simply do not feel right. Scientists have already achieved success in creating flexible prostheses that restore some normal functions. These devices typically determine electrical signals from the muscles above the point of amputation using surface electrodes — a non-invasive approach, but less selectively affect individual nerve fibers.
“Figuratively speaking, it’s just as difficult to have a private conversation with someone inside a football stadium if you shout outside,” said George.
Later prostheses are connected directly to the source: the patient's motor cortex or its remaining nerves in the cult. These nerves convey the intent of the brain to move to an amputated limb, these signals can be decoded to move the prosthetic arm.
Compared to the brain, the nerves of the hands are much safer to implant. Their signals are also easier to understand - one neuron gives a signal, one muscle is twitching. Instead of trying to determine the signal among the cacophony of the cerebral cortex, it makes much more sense to act downstream.
However, despite the amazing technology that allows patients to control the robotic arm with thought, these devices still have problems.
Without the sensory feedback we usually get, patients cannot fine-tune grip. Instead of pinching grapes, they end up turning it into a porridge. It is not intuitive and frustrating.
“As a result, almost 50 percent of patients refuse prostheses. We want to restore the full experience of using the hand, ”says George.
 Roboruka allows Kevin to feel the objects again, he could take grapes without crushing the berries. (University of Utah)
Roboruka allows Kevin to feel the objects again, he could take grapes without crushing the berries. (University of Utah)Utah Decision
 Researchers at the University of Utah have developed technology that allows users to sense objects with a robotic arm. In one experiment, they were able to distinguish a soft sponge from hard plastic.
Researchers at the University of Utah have developed technology that allows users to sense objects with a robotic arm. In one experiment, they were able to distinguish a soft sponge from hard plastic.
The work of the new system consists of two parts: first, it picks up signals from the brain through two microelectronic arrays into a fraction the size of a penny, which are implanted in the patient's residual nerves that excite the arm. At the same time, another part of the electrodes picks up signals from the residual muscles.
“After implantation, we have to create a map of what sensations are possible, and this is individual for each patient,” says George.
We carefully stimulated each of the electrodes of the array, for a total of 192, and asked Kevin to report where he felt and how it felt.
For example, electrode 64 was associated with a feeling of pressure on a fingertip. The team activates a pressure sensor on the thumb of the prosthesis, so that it behaves like a biological arm.
As soon as we complete the mapping, the entire translation process happens automatically. Kevin can intuitively move a prosthetic hand as if controlling his own hand.
When the prosthesis makes contact, the team stimulates the corresponding electrode to provide feedback to the patient. For a fingertip, this is electrode 64. The stronger the pressure, the stronger the signal. In essence, electrode arrays essentially replace lost nerve endings, which usually excite a hand.
Thus, when the thumb of the prosthesis touches the grapes, Kevin feels the touch.
The functional improvements were huge. In one test, where Kevin was asked to move around a “mechanical egg” that feels pressure, he achieved success without breaking the boundary, and showed a result 21% better when sensory feedback was turned on.
Whole me
But perhaps the biggest advantage is emotionality.
In one
video, the former participant was asked to touch the virtual door with a computer prosthesis. The simulation was cartoony and rough, but it didn't matter to the patient.
Reaching out to the door, he sighed loudly: “Oh my God. I feel the door! ”And exclaimed, gasping:“ God! That is so cool!"
“The point is not that the participant felt the touch with his missing hand, the fact is that he felt the door for the first time in 24 years of interaction with the external environment,” explains George.
This feeling is the embodiment of what was previously absent in prosthetics.
Kevin's experience was no less cunning. After training with a prosthetic arm printed on a 3d printer, he was asked what he would like to do?
“I want to squeeze my hands together,” he said, folding the rest of his hand into a loose fist, gently, repeatedly pressing against the prosthesis, as if massaging the knuckles after a long day.
“Initially, the prosthesis was just a tool to help him with activities in everyday life, but now, this is what behaves like his own hand.
It is not only about improved dexterity or improved sensitivity, but also about feeling one again, ”George.
The team is now enthusiastically working on a wireless home version of their patient system to use in everyday life. Without wires, you should have less chance of infection and breakage. It is also expected that these benefits will increase with increasing practice and continued use.
Having already tested the current interface with seven patients, the team feels confident. They say they will make a wireless version, ready for human testing in about a year.
“Ultimately, as one of our patients said, it will look just like the hand of Luke Skywalker, then everyone will want such a prosthesis,” concludes George with a broad grin.
 The arm "Luke", a robotic prosthesis created by DEKA and named after Luke Skywalker, the hero of Star Wars, who wore a prosthesis.original
The arm "Luke", a robotic prosthesis created by DEKA and named after Luke Skywalker, the hero of Star Wars, who wore a prosthesis.originalIf you want to join the development or you have ideas on the mechanism, construction, design of the prosthesis, use experience, we invite you to our working
chat . We continue the discussion in the format of a dialogue.